The Infection Prevention and Control Unit
Mycetoma Research Centre (MRC), University of Khartoum
WHO Collaborating Centre on Mycetoma and Skin NTDs
Healthcare-associated infections (HAIs) remain one of the most frequent adverse events in healthcare delivery, negatively affecting patient outcomes, increasing morbidity, prolonging hospital stays, and placing an additional financial burden on health systems. In low- and middle-income countries, up to 10% of patients acquire at least one HAI, a significant proportion of which can be prevented through well-structured infection prevention and control (IPC) programmes.
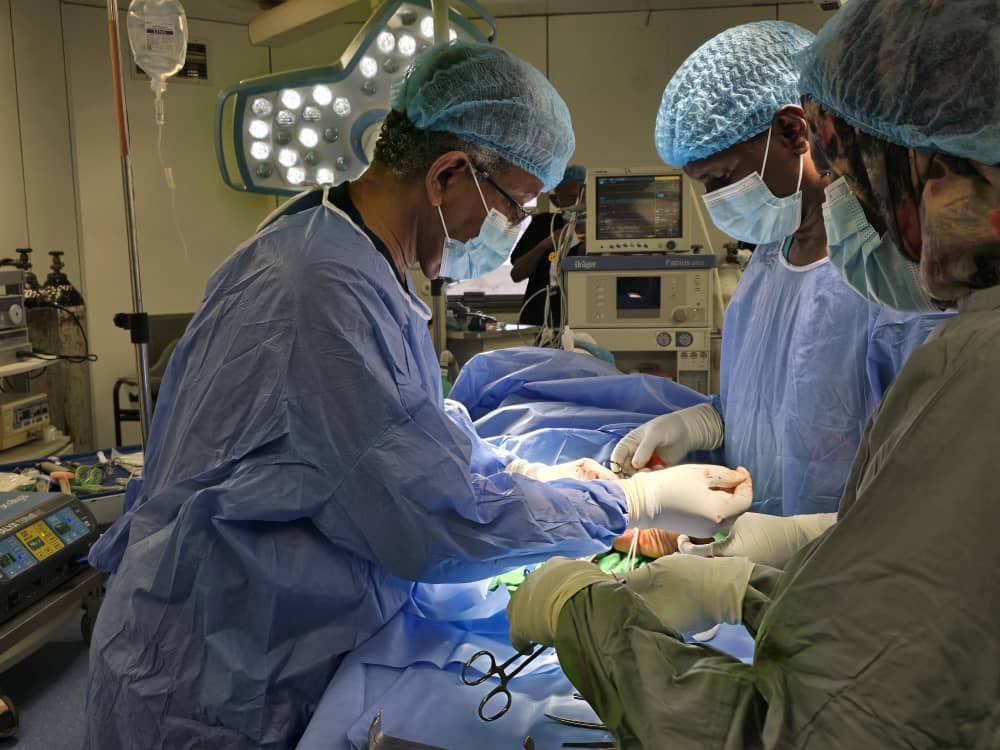
The Mycetoma Research Centre (MRC) is internationally recognised for its leadership in mycetoma care, scientific research, training and community engagement initiatives. It manages patients with complex, chronic infections that often require repeated surgical interventions and prolonged antifungal and antibacterial treatments. Such clinical activities inherently increase the risk of surgical site infections, cross-transmission of infectious agents, occupational exposure among healthcare workers, and the emergence of antimicrobial resistance.
The World Health Organization underscores the importance of establishing dedicated IPC programmes in all healthcare facilities, supported by trained personnel, effective surveillance systems, and clear standard operating procedures to ensure patient and staff safety.
Justification
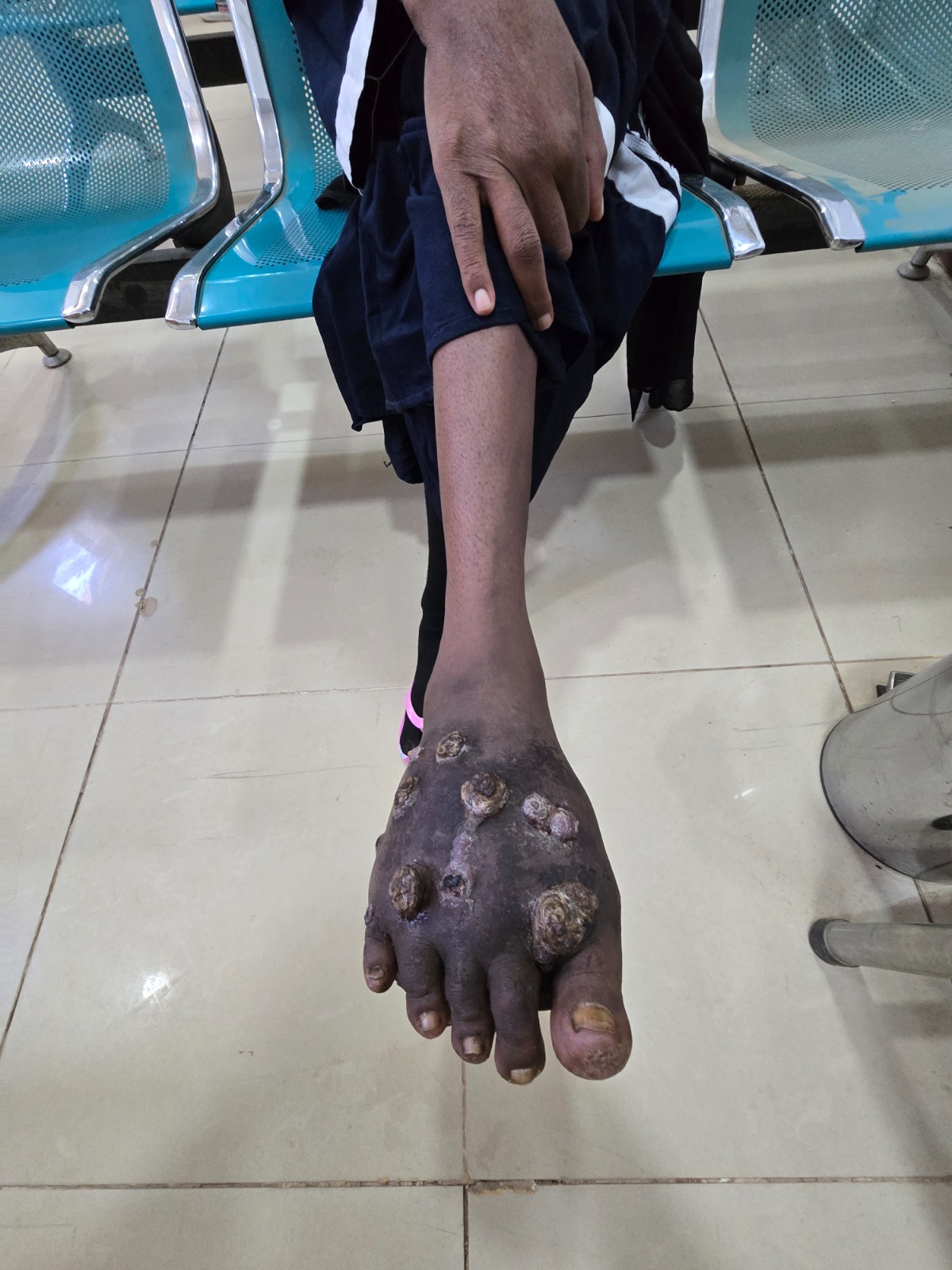
Establishing an Infection Prevention and Control (IPC) Unit at the Mycetoma Research Centre (MRC) is both necessary and strategic. From a clinical perspective, patients with mycetoma frequently present with chronic open lesions and often require repeated surgical interventions, which significantly increases the risk of infections. In addition, prolonged antimicrobial therapy heightens the risk of antimicrobial resistance, while effective prevention of healthcare-associated infections contributes to better treatment outcomes and fewer complications.
From a public health standpoint, IPC programmes play a critical role in reducing the transmission of infections within healthcare facilities and into the wider community. They also strengthen preparedness and response to outbreaks and emerging infectious threats.
At the institutional level, establishing an IPC Unit will further reinforce MRC’s standing as a WHO Collaborating Centre, while ensuring alignment with international accreditation requirements and patient safety standards. It will also contribute to improving the overall quality of care and strengthening patient confidence in the services provided.
Economically, effective IPC measures help reduce costs associated with prolonged hospital stays, repeat surgical procedures, and the management of complications. By focusing on prevention, resources can be utilised more efficiently.
Importantly, there is strong evidence supporting the impact of IPC programmes, with healthcare facilities that implement structured IPC systems and employ trained personnel demonstrating substantial reductions in infection rates, often by 30% or more.

Objectives
- Develop and implement a comprehensive IPC programme.
- Establish surveillance systems for HAIs.
- Strengthen infection prevention practices across all departments.
- Promote rational antimicrobial use and combat AMR.
- Ensure a safe environment for patients, staff, and visitors.
- Build capacity through continuous education and training.
Core Functions of the IPC Unit
Based on WHO core components and best practices, the IPC Unit:
- Develop policies and guidelines (standard and transmission-based precautions).
- Conduct HAI surveillance and reporting.
- Implement infection prevention measures (hand hygiene, PPE, sterilisation).
- Monitor environmental cleaning and disinfection.
- Train healthcare workers.
- Ensure occupational health and safety.
- Support outbreak preparedness and response.
- Promote antimicrobial stewardship.
The Actions of the Infection Prevention and Control Unit
The Infection Prevention and Control (IPC) Unit will undertake a set of coordinated administrative, technical, capacity-building, and monitoring actions to ensure effective implementation of infection prevention standards across the Mycetoma Research Centre.
At the institutional and administrative levels, the Unit will lead the development and ongoing updating of IPC policies and guidelines in alignment with World Health Organisation recommendations. It will advocate for and secure the necessary resources, including dedicated budget lines, qualified personnel, and appropriate infrastructure to support IPC activities. In addition, the Unit will facilitate the establishment and functioning of an Infection Control Committee to provide strategic oversight and multidisciplinary coordination.
From a technical perspective, the Unit will develop and implement standard operating procedures (SOPs) tailored to the specific needs of mycetoma care and clinical services at the Centre. It will establish and maintain robust infection surveillance systems to monitor healthcare-associated infections and identify trends. Furthermore, the Unit will play a central role in developing and operationalising an antimicrobial stewardship programme to promote the rational use of antimicrobials and reduce the risk of antimicrobial resistance.
Capacity building will be a core function of the Unit, with regular training programmes designed to equip healthcare workers with the knowledge and skills required for effective IPC practice. This will include structured orientation for new staff as well as ongoing continuous professional development initiatives to ensure sustained competency and adherence to best practices.
Monitoring and evaluation activities will be integral to the Unit’s work. Regular audits and assessments will be conducted to evaluate compliance with IPC standards across all departments. The Unit will systematically monitor adherence to key practices, including hand hygiene, the use of personal protective equipment, and environmental cleaning. Based on these assessments, timely feedback will be provided to departments, along with corrective actions to address gaps and improve overall performance.
Key Activities
| Policy and Guidelines | Developed mycetoma care IPC manual
|
| Standardise protocols development | Hand hygiene
PPE use Sterilisation and disinfection Waste management
|
| Surveillance | Established HAI surveillance system.
|
| Monitor | Surgical site infections
Wound infections Laboratory-confirmed infections
|
| Training and Education | Regular training workshops for staff
Orientation for new staff and students Community awareness programmes.
|
| Environmental Control | Ensure proper cleaning and disinfection protocols
Monitor water, ventilation, and waste systems Implement safe construction and renovation practices
|
| Occupational Health | Vaccination programs for staff
Post-exposure prophylaxis protocols Regular health screening
|
| Antimicrobial Stewardship | Monitor antimicrobial use
Develop treatment guidelines Promote rational prescribing
|
| Outbreak Preparedness | Develop outbreak response plans
Rapid detection and containment systems
|
Organisational Structure
Infection Prevention and Control Committee
A multidisciplinary committee responsible for governance and strategic direction.
Members include:
- Director of MRC (Chair)
- IPC Unit Head
- Microbiologist
- Surgeon
- Pharmacist
- Nursing representative
- Laboratory representative
- Public health expert

The IPC Unit Team
| IPC Director | Oversees programme implementation and strategy
|
| Infection Control
Physician
|
Clinical oversight and policy development
|
| Infection Control
Nurses |
Day-to-day implementation and monitoring |
| Microbiologist | Laboratory support and surveillance
|
| Pharmacist | Antimicrobial stewardship
|
| Environmental Health Officer
|
Cleaning, waste management, and facility safety |
| Data Manager / Surveillance Officer | Data collection, analysis, and reporting |
| IPC coordinator | Facilitate communication and compliance at the unit level
|
Reporting and Integration
- IPC Unit reports directly to MRC leadership.
- Integrated into:
- Clinical services
- Research activities
- Training programs
Infection control must be embedded across all institutional systems, not isolated as a standalone activity.
Monitoring and Evaluation Indicators
- HAI rates (e.g., surgical site infections)
- Hand hygiene compliance
- PPE adherence rates
- Antimicrobial usage patterns
- Staff training coverage
- Audit and inspection results
