Cutaneous tuberculosis mimicking a mycetoma; a case report
Eiman Siddig, Ahmed Hassan Fahal
The patient is a 50-year-old female, a primary school teacher from Gezira State, who presented to the Mycetoma Research Center, University of Khartoum, Khartoum, Sudan, with painful swellings in her left foot. Her condition started one year prior to presentation with pain at the lateral malleolus, then a mass appeared which was one centimeter in diameter, and eventually, a sinus discharging blood and pus developed. She was seen at a local health center, and a wide local excision was done under local anaesthesia, which was diagnosed as a cyst.
In the recent presentation, she had recurrent painful swelling at the lateral malleolus with an extension to the medial malleolus. Both swelling had sinuses discharging pus and blood. Although she had mild pain, this didn’t prevent her from undertaking her normal daily activities and pursuing her teaching career until recently. She recalls no history of trauma, family history of mycetoma or similar condition. However, she underwent amputation of her small left finger due to a foreign body that she had previously neglected. She has no chronic illness and is not on long-term medications. She is from a mycetoma endemic area. Her past medical, social, geographical or gynaecological is not contributory to her present condition.
Clinically she looked well, not pale nor jaundiced. She was orientated and cooperative. The patient was vitally stable. General systematic clinical examinations were within normal. A local foot examination revealed a left lateral calcaneal ulcerating swelling and another one on the medical side. There were a few sinuses around the lesions on both sides. The lesions had pusy offensive bloody discharge. The lesions’ edges were slightly raised, and the surrounding skin was oedematous. No grains were seen, and there was no regional lymphadenopathy. The lower limb was within normal. (Figs. 1,2).


Her general laboratory investigations showed haemoglobin of 13.8g/dl, a normal total white blood cells count of 5.98 /dl, and a normal platelets count. The renal function test was normal, with urea of 20 mg/dl and creatinine of 0.9 mg/dl.
She underwent an ultrasound investigation of the left foot, which revealed turbid fluid collection measuring about 5.3*6.7 cm in diameter, mostly representing inflammatory collection and extensive superficial soft tissue oedema. (Fig. 3)
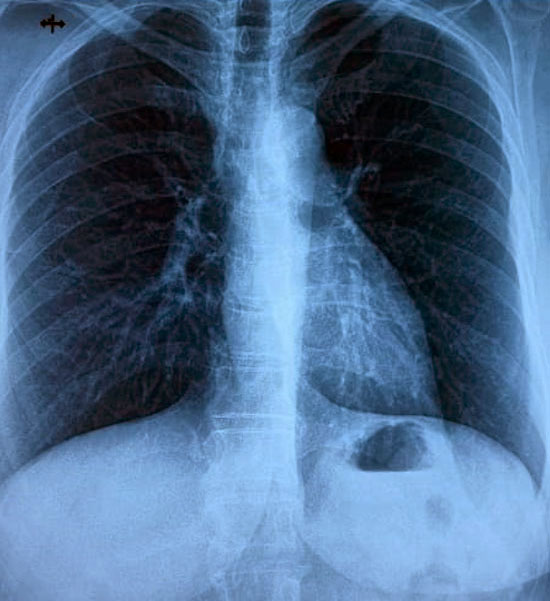
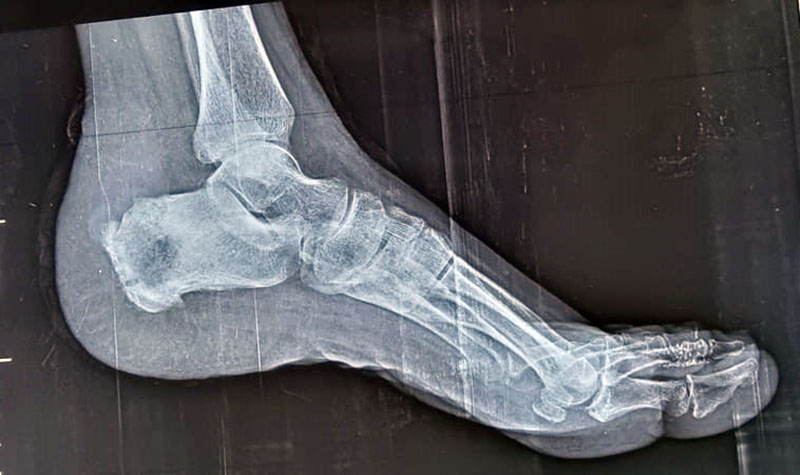
Left foot X-ray in the lateral and anteroposterior views showed soft tissue swelling and cavitation at the calcaneus bone (Fig.4). Her chest x-ray showed no abnormality.
Fine needle aspirations for cytology were done. The smears examinations revealed severe active chronic inflammation evidenced by heavy mixed inflammatory cells, spindle, stromal cells, fat cells and RBCs on the smear.
She underwent wide local excision and bone curettage of the two lesions under spinal analgesia. Bone curettage showed whitish gelatinous material. There was no bone communication between the two cavities. The surgical biopsy showed evidence of tuberculous osteomyelitis.
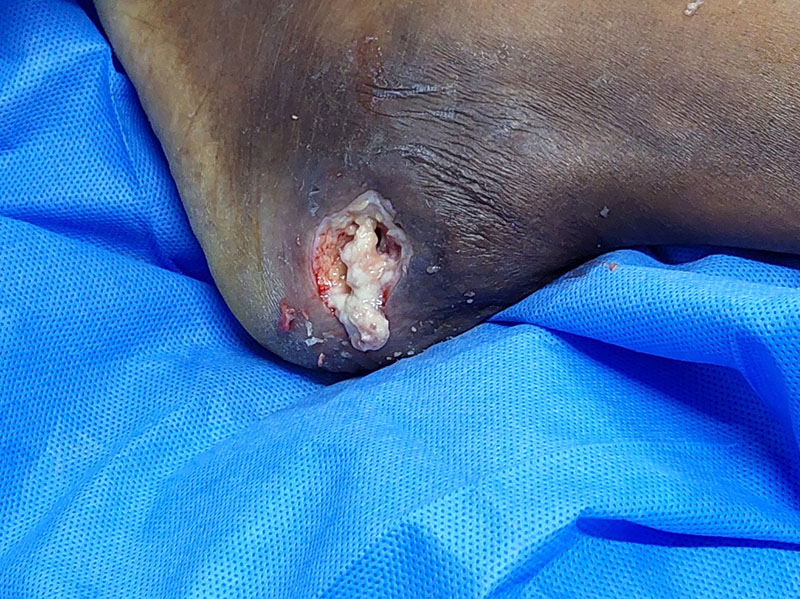
She had an uneventual postoperative recovery and was referred to the medical Department for antitubercular treatment.
Learning Points
- Tuberculous osteomyelitis is a rare condition but should be considered in the differential diagnosis of mycetoma.
- Pain is not a common feature of mycetoma or tuberculosis
- The bone changes in both conditions are almost similar.
